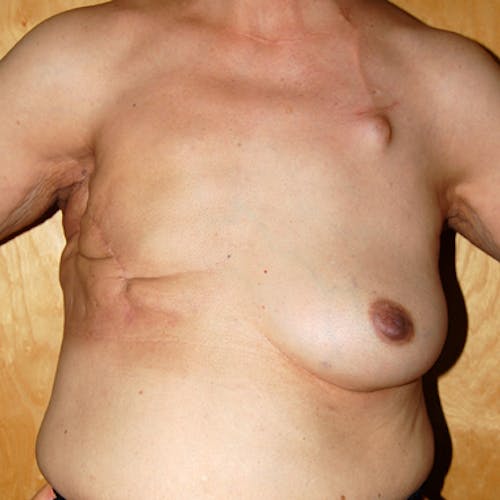
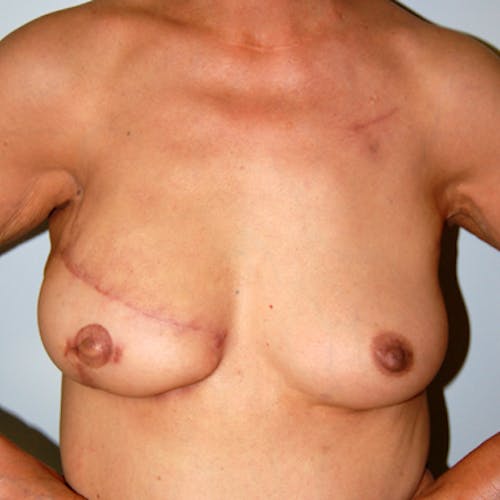
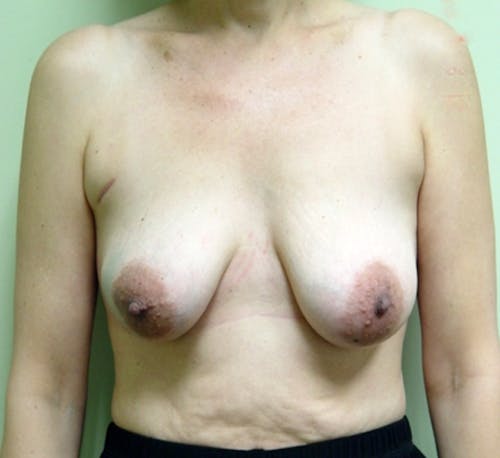
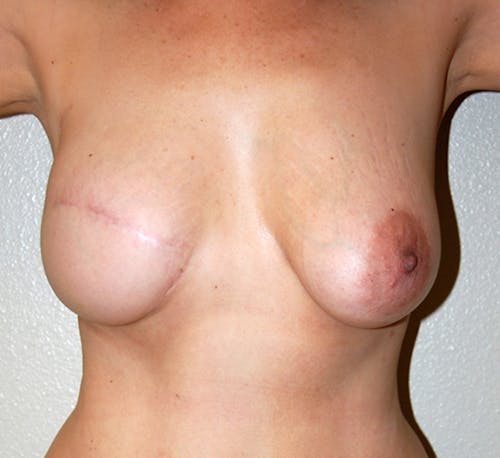
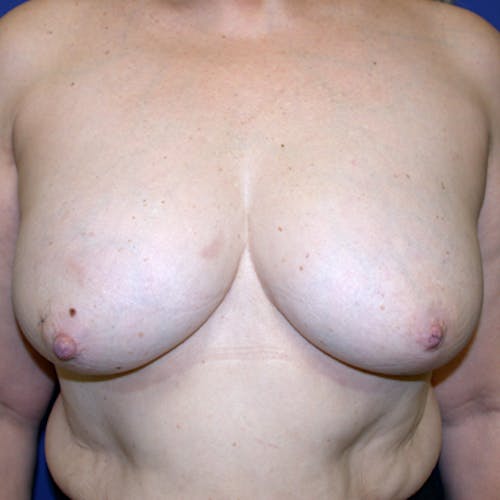
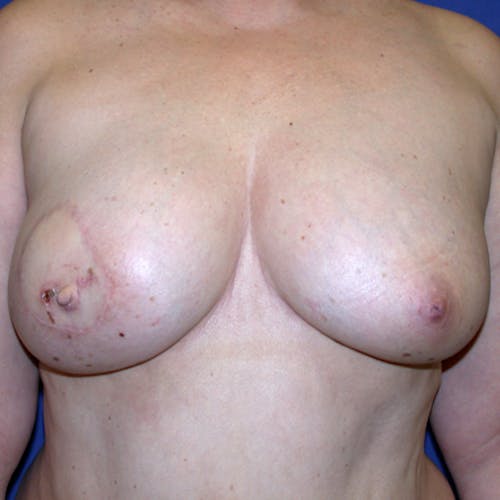
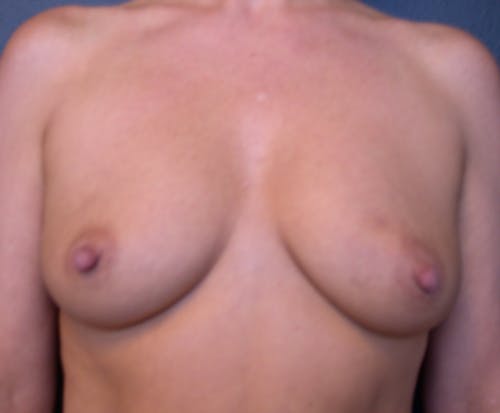
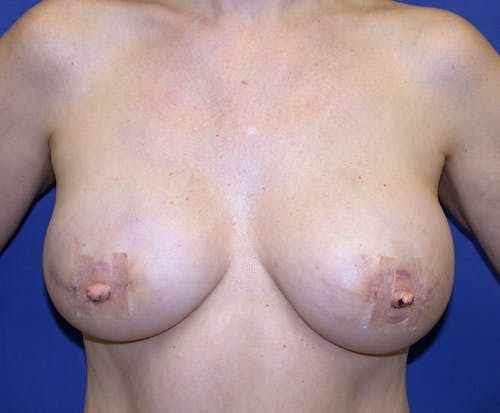
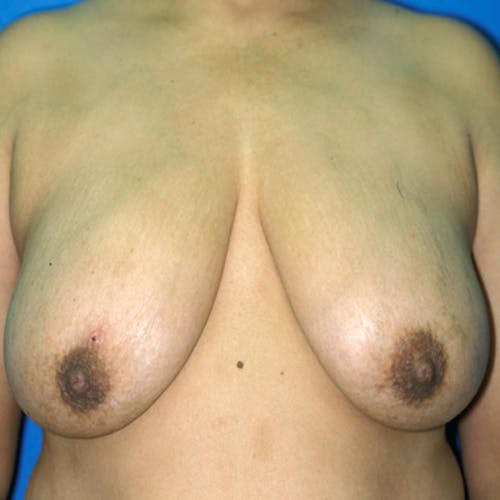
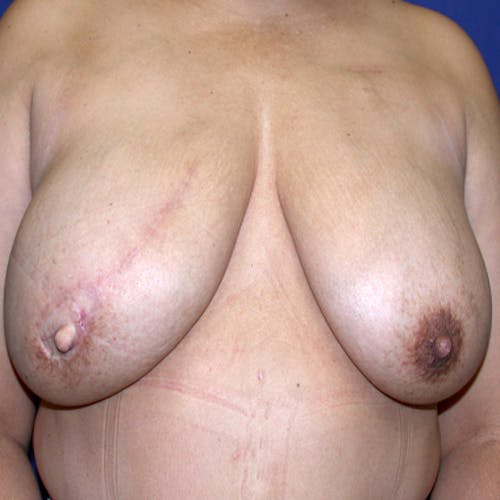
These complex reconstruction methods are used when implant reconstruction is not enough, or if you simply prefer to use your own tissue to reconstruct your breast mound.
TRAM & DIEP Flap Reconstruction Frequently Asked Questions
Will I lose abdominal strength with TRAM or DIEP?
In some cases, yes. TRAM involves removing some abdominal muscle, which can affect your core strength. DIEP spares your muscle, which preserves function and reduces your future hernia risk.
Can a TRAM or DIEP flap be combined with an implant?
Yes, in select cases. If you need additional volume, Dr. Gupta may be able to combine a TRAM or DIEP flap with an implant beneath the transferred tissue. This hybrid approach merges your soft natural tissue with the structure of an implant.
Will the results be permanent?
Because Dr. Gupta uses vascularized tissue for this reconstruction, you can expect extremely long-lasting results. With that said, future weight changes or pregnancies will impact your breasts.
How does Dr. Gupta minimize abdominal weakness with the TRAM flap?
Dr. Gupta carefully tailors each San Diego TRAM flap surgery to preserve as much muscle as possible. He reinforces the donor site using specialized mesh when needed and reattaches the remaining muscle layers to maintain your core strength.
What happens if I’ve had a previous abdominal surgery or C-section?
A previous abdominal procedure doesn’t necessarily rule out a TRAM flap. Before surgery, Dr. Gupta will evaluate your abdominal wall and blood vessel anatomy via imaging. In some cases, he may modify the flap design or recommend an alternative approach, such as a latissimus flap or DIEP reconstruction, to ensure a successful outcome.
How long does a TRAM or DIEP flap last?
Once you’ve healed from surgery, the flap tissue becomes part of your body. It ages and changes with your weight, just like natural breast tissue. Unlike implants, you won’t need to replace this tissue in the future.